Every year, millions of patients wait weeks for test results that could save their lives. Doctors miss early signs of cancer because they’re overwhelmed. Hospitals run out of staff, and critical decisions are made under pressure. But something is changing - quietly, powerfully, and already saving lives. Artificial intelligence isn’t just another tech trend. It’s becoming the invisible second opinion in every hospital, clinic, and lab around the world.
AI Sees What Human Eyes Miss
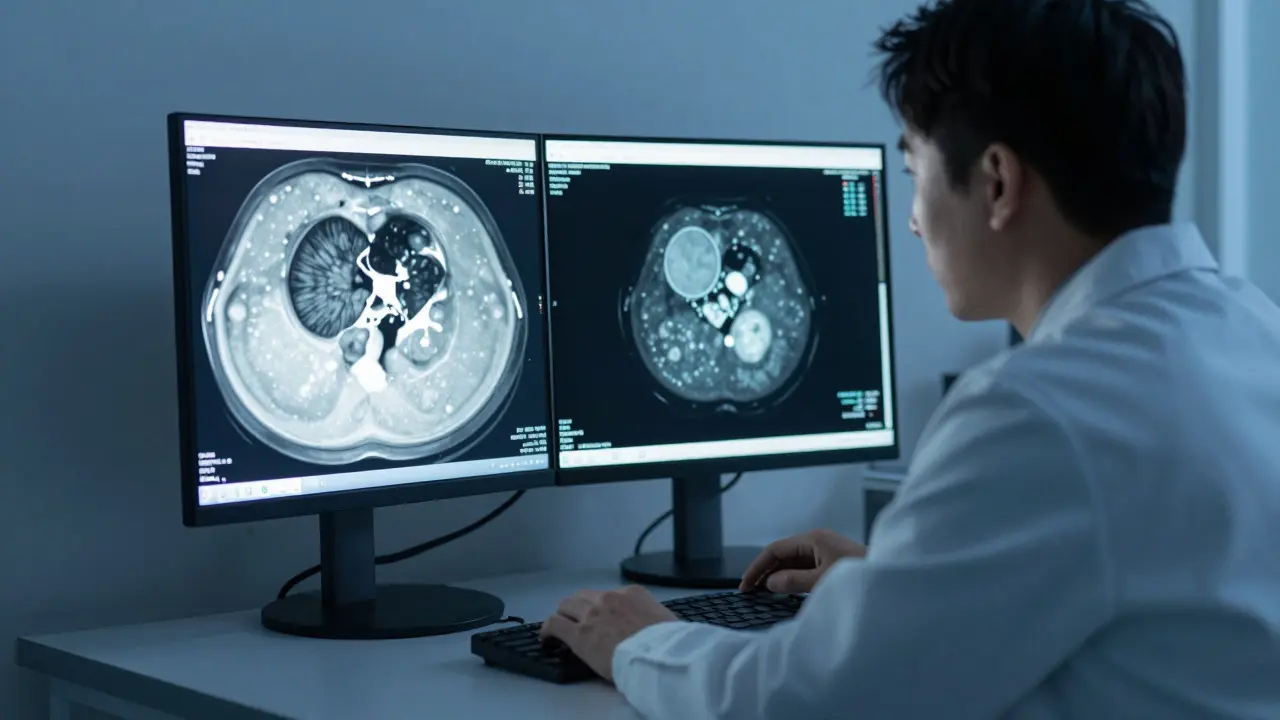
In radiology, a single CT scan can generate hundreds of images. A radiologist might spend 15 minutes reviewing one scan. That’s fine - until they have to do 50 of them in a day. Fatigue sets in. Subtle tumors, tiny bleeds, or early signs of stroke can slip through. That’s where AI steps in.
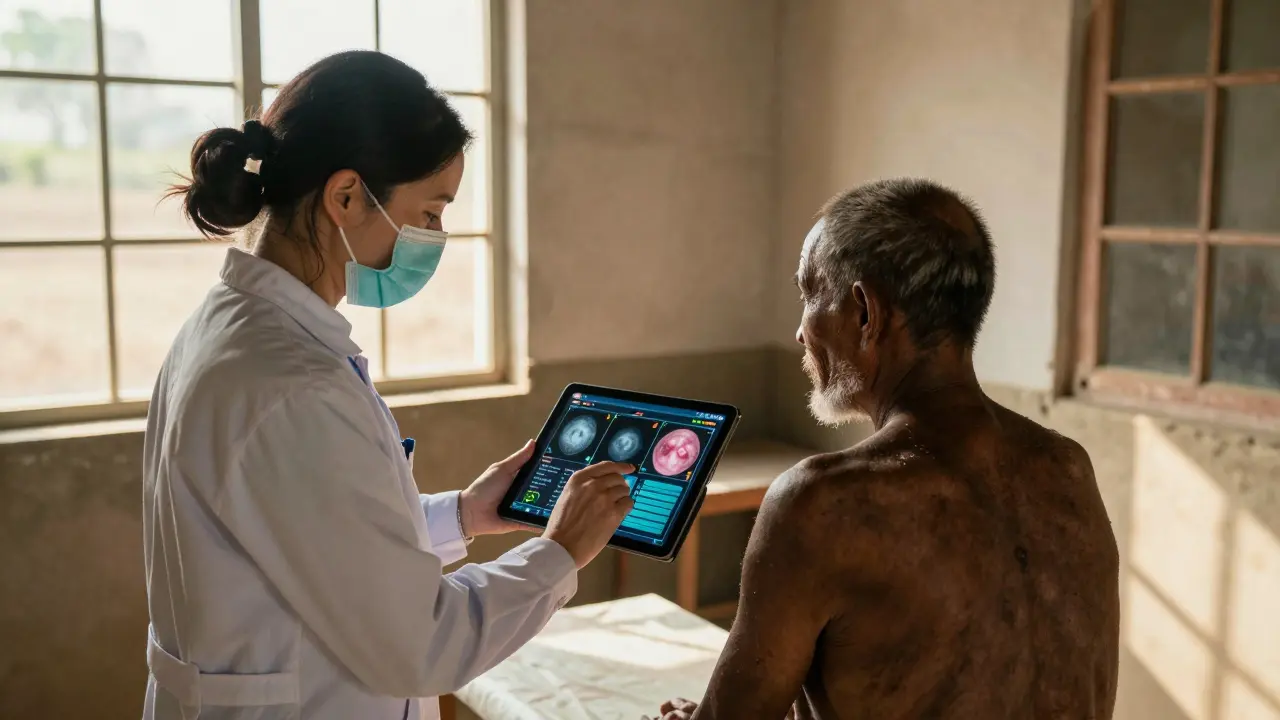
Google’s DeepMind developed an AI model that analyzes retinal scans for signs of diabetic retinopathy. In trials, it matched the accuracy of top eye specialists. In rural clinics in India and Kenya, where ophthalmologists are rare, this AI now flags high-risk cases before a human ever sees them. It doesn’t replace doctors. It gives them a second pair of eyes - one that never blinks, never tires, and never misses a pattern.
Similarly, AI tools trained on millions of mammograms can detect breast cancer up to 11 months earlier than traditional methods. A 2025 study from the Mayo Clinic showed AI reduced false negatives by 37% and cut radiologist workload by 44%. That means more lives caught early - and fewer unnecessary biopsies for women who don’t have cancer.
Speeding Up Diagnosis, Saving Lives
Time is everything in emergency medicine. When someone arrives with chest pain, every minute counts. AI-powered systems now analyze ECGs in under 10 seconds. In one Australian hospital in Hobart, an AI tool flagged a rare heart rhythm disorder in a 42-year-old man who thought he just had indigestion. By the time the cardiologist arrived, the system had already alerted the team: he needed immediate intervention. He’s now back at work.
These aren’t lab experiments. Real hospitals are using them. At Johns Hopkins, AI predicts sepsis - a deadly bloodstream infection - up to 12 hours before symptoms appear. It watches hundreds of vital signs: temperature, heart rate, blood pressure, oxygen levels, even lab results. When it spots a pattern that matches past sepsis cases, it alerts nurses. The hospital’s sepsis mortality rate dropped by 20% in six months.
AI doesn’t just react. It predicts. In neonatal units, it monitors premature babies’ breathing patterns and predicts apnea episodes before they happen. In intensive care, it forecasts which patients are likely to need a ventilator in the next 24 hours. That lets staff prepare - instead of scrambling.
Personalized Treatment, Not One-Size-Fits-All
Cancer treatment used to mean chemotherapy, radiation, or surgery - the same options for everyone with the same diagnosis. But tumors aren’t identical. Two people with ‘lung cancer’ might have completely different genetic mutations driving their disease.
AI now analyzes a patient’s tumor DNA, lifestyle, medical history, and even gut microbiome to recommend targeted therapies. In Australia, the Peter MacCallum Cancer Centre uses AI to match patients with clinical trials they’d otherwise never be offered. One woman in her 50s, told she had no options left, was matched with an experimental drug based on a rare mutation. Two years later, she’s cancer-free.
For chronic diseases like diabetes or heart failure, AI builds personalized care plans. It tracks glucose levels, activity, sleep, and medication adherence - not just from wearables, but from hospital records, pharmacy data, and even text messages. It learns what works for *this* person, not the average patient. Adjustments happen automatically. No more waiting for a monthly check-up to fix what went wrong last week.
AI Is Cutting Costs - and Reducing Burnout
Hospitals spend nearly 30% of their budget on administrative tasks: scheduling, billing, insurance claims, paperwork. Nurses spend more time on computers than on patients. AI is changing that.
Chatbots now handle 60% of routine patient inquiries - appointment changes, prescription refills, post-op instructions. In the U.S., a hospital in Ohio cut call center costs by $1.2 million a year using AI chatbots. In Australia, AI transcribes doctor-patient conversations in real time and auto-fills electronic health records. No more typing after a 12-hour shift. Doctors report feeling heard again.
AI also predicts staffing needs. By analyzing patient flow, seasonal trends, and even weather patterns (yes, flu spikes after cold snaps), it tells managers when to schedule extra nurses. One Melbourne hospital reduced overtime costs by 22% and cut patient wait times by 38% in just four months.

Challenges - And Why We Can’t Ignore Them
AI in healthcare isn’t perfect. Bias is a real problem. If an AI is trained mostly on data from white, middle-class patients, it may miss signs of disease in Black, Indigenous, or low-income populations. A 2024 study found that some AI tools were 30% less accurate in diagnosing skin cancer on darker skin tones.
That’s why hospitals now demand transparency. They ask: Where did the data come from? Who built it? Was it tested on diverse groups? The FDA now requires AI tools to prove they work across race, gender, and age before they’re approved for hospitals.
Privacy matters too. Your medical data is sacred. AI systems must be built with strict encryption, anonymization, and clear rules on who can access the data. In Australia, strict laws like the Privacy Act 1988 and the My Health Record system ensure AI tools follow the same rules as human doctors.
And yes - some fear AI will replace doctors. But the truth is, it’s doing the opposite. It’s freeing them from paperwork, giving them better tools, and helping them focus on what matters: the person in front of them.
The Future Is Already Here
Imagine a world where your wearable alerts your doctor before you even feel sick. Where AI scans your blood test results and spots a rare autoimmune marker no human would notice. Where a child with epilepsy gets a custom treatment plan built from 10,000 similar cases - and it works.
This isn’t science fiction. It’s happening now. In rural clinics in Tasmania. In urban hospitals in Sydney. In research labs in Melbourne. In the U.S., Europe, and Africa.
AI won’t cure every disease. But it’s making healthcare faster, fairer, and more personal. It’s not about replacing humans. It’s about giving them the power to do what they do best - care.
Can AI replace doctors?
No. AI doesn’t replace doctors - it empowers them. It handles repetitive tasks like analyzing scans, predicting risks, and sorting data. That frees doctors to focus on complex decisions, patient communication, and emotional support. The best outcomes happen when AI and human judgment work together.
Is AI in healthcare safe?
Yes - if it’s built and tested properly. Leading AI tools undergo strict clinical validation before being used in hospitals. They’re tested on diverse populations to avoid bias, and they’re monitored continuously for errors. Regulatory bodies like the FDA and Australia’s TGA require proof of safety and accuracy. Still, no system is perfect, which is why human oversight remains essential.
How is AI improving access to care in remote areas?
In places with few specialists, AI acts as a force multiplier. A nurse in a rural clinic can use an AI-powered app to scan a skin lesion and get an instant risk assessment. A portable ultrasound device with AI guidance can help diagnose heart issues without a radiologist on-site. In Australia’s Outback, these tools have cut diagnosis delays by over 70%.
What data does AI use to make decisions?
AI systems use a mix of data: medical images (X-rays, MRIs), lab results, electronic health records, wearable device data (heart rate, sleep), genetic information, and even patient-reported symptoms. The key is that the data must be high-quality, diverse, and ethically sourced. Hospitals now audit AI training data just like they audit medications.
Are AI tools expensive for hospitals to adopt?
Some are, but many aren’t. Cloud-based AI tools now cost less than $10,000 per year to implement - far less than hiring an extra radiologist. Many tools pay for themselves in under a year by reducing errors, cutting administrative costs, and preventing costly complications. Smaller clinics can use affordable AI plugins that work with existing systems like Epic or Cerner.